It is a silent thought, a thought that hardly a person speaks about at a certain point in life:
“I’m not good enough.”
It does not necessarily come in the form of a theatrical meltdown or a high-volume self-doubting situation. In practice more frequently it creeps in unobtrusively and presents itself as an outwardly productive or responsible behavior. It can present itself as overworking to demonstrate its value, people-pleasing to evade rejection, procrastination because of fear of failure, or a general worry of being found out as a scammer even when it can be seen that it is capable.
Otherwise, this thought is veiled with perfectionism or self-criticism that is initially feels encouraging to you, as it drives you to perform better, exert more, be better. However, as time goes, this internal pressure gradually destroys the self-worth, and in its place, the confidence is substituted with fatigue and the trust in self is substituted with doubt.
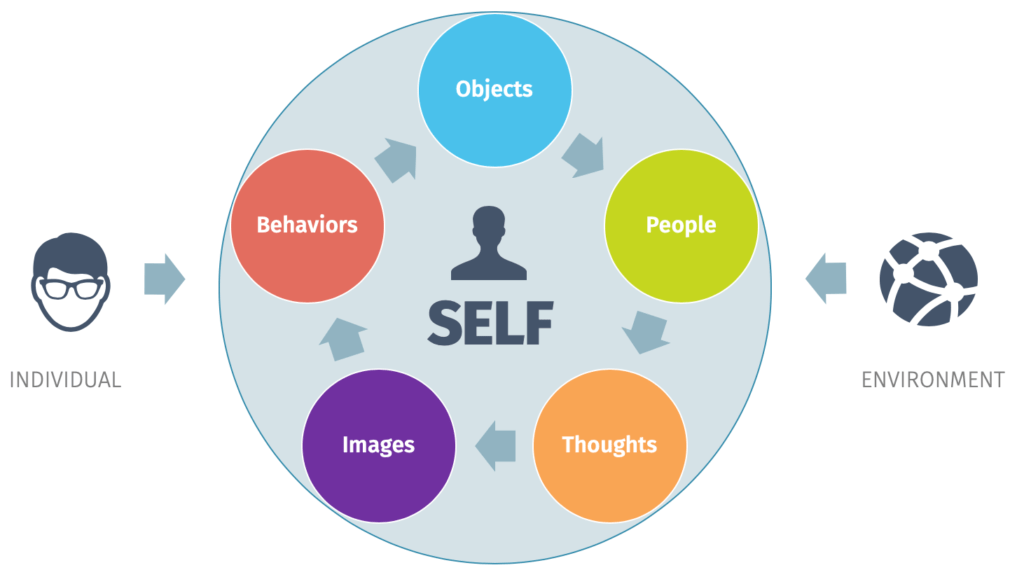
The point to note is that, the experience of not being good enough is not an individual failure or character flaw. It is a mental process, a pattern, and in most cases, these patterns were formed in early age and reinforced by experience, relationships and social expectations and misinterpreted as a lack of confidence or competence.
In order to remedy it, we must go beyond outward conduct and self-occurrence and have a look at what is occurring under the surface.
1. “Not Good Enough” Is Rarely About Ability
There are numerous individuals who find themselves battling the sense of incompetence but in actuality, they are capable, intelligent, and emotionally competent. They may possess abilities, competence, and even external authentication, but people feel like they are not good enough. The reason is that it is not often a failure in capability. Rather it is the way the brain has been conditioned to assess safety, belonging and self worth.
Psychologically, competence is not the main concern of the mind. It is preoccupied with survival.
So it doesn’t ask:
-
“Am I capable?”
-
It asks:
-
“Am I safe, accepted, and valued?”
Once the acceptance, particularly during initial relationships, is perceived as conditional, then the brain will start identifying value as performance. Love, approval or attention are something one feels deserved not innate. This builds within it an internal perception that one needs to prove, achieve or live up to expectations in order to be valued.
Subsequently, even competent people can be left constantly feeling under competent not due to their ineptitude, but simply because their nervous system was taught that it is necessary to earn a place by performance.
2. Conditional Love and Early Programming
Among the most potent and the most neglected sources of inadequacy feeling is the conditional validation through childhood. As long as care, love, or emotional security was tied to some behavior, performance or emotional control, then the growing nervous system learned to tie love to performance.
Depended on when love, attention, or praise is required:
- being well-behaved
- achieving results
- meeting expectations
- not communicating hard, troublesome, and awkward feelings.
the child did not consciously believe that there is something wrong with the environment. Rather the mind evolved by creating a strong internal law:
I am supposed to be worthy when I do something right.
This conviction is not instilled in the mind, but in the nervous-system system. It sets an internal score board that never stops running – it measures behavior, tracks reactions and assesses whether one is doing enough to remain accepted.
The brain still searches to find indicators of approval or disapproval even in adulthood when the original environment is no longer the same:
- Did I say the right thing?
- Was I impressive enough?
- Did I disappoint someone?
This self-monitoring constantly is mistaken with insecurity or having low confidence. Or, more accurately, it is survival learning the system which is created to preserve connection preventing the emotional loss.
3. The Inner Critic Is a Protective Voice, Not an Enemy
That terrible voice within that says:
- “You should be better.”
- “Others are ahead of you.”
- “Don’t mess this up.”
is usually weighted down with misunderstanding. The majority efforts are making it silent, arguing with it or being ashamed to have it at all. Yet psychologically, the critic within did not evolve to your detriment, he evolved to your advantage.
The inner critic develops in early life as a defense against rejection, shame, punishment or failure. It thinks that, through keeping you alert, self-critical and striving at all times, it can assist you to escape emotional pain. To its reasoning, pressure is safety.
In the eyes of the nervous system, criticism is safer than getting taken unawares.
The issue does not lie in the presence of the inner critic. The problem is that:
- it never renews its strategy.
- is not aware that things have changed.
- it knows not when you are now more familiar, more mature, more able.
So it proceeds to push, threaten and squeeze tighter- even after the real threat has passed. What at one time served to sustain your life now holds you in the fear, self-doubt and emotional exhaustion.
The process of healing does not start by fighting with the inner critic, but by knowing the reasons behind why it had learnt to talk that way in the first place.
4. Social Comparison Hijacks the Brain
The contemporary world makes inadequacy feelings significantly heavier with social comparison at all times. Although comparison is a common human behavior, the brain has never been created to handle the magnitude and frequency of occurrence of the act today.
The development of the human brain was such that it was developed to compare itself in small and familiar groups where context, mutual struggle and real life interactions could be seen. To-day however, the brain is expected to compare:
- your behind-the-scenes life
- and highlights of other people carefully edited.
- This disproportion fills the nervous system.
Instead of causing motivation or development, constant comparison leads to the brain turning on the system of threat-detection that uses the same mechanism that identifies danger. When the brain thinks of others as being in front, it fails to give it out as a neutral information. It interprets it as risk.
Comparison results in most cases in lieu of inspiration:
- shame
- self-doubt
- emotional apathy or closure.
A more profound level of interpretation of a fall behind by the brain is that it is a possible loss of belonging. And to a social nervous system, to lose belonging is very unsafe, almost the danger of being killed.
That is why comparison does not only damage confidence; it causes a disturbance in the emotional security.
5. Trauma and Emotional Neglect Amplify the Belief
The second belief is that I am not good enough, which is particularly widespread in the group of people who experienced in their childhood:
emotional neglect
variable or irregular care giving.
chronic criticism
minor nullification of feelings, needs or perceptions.
In such settings, lack of emotional sensitivity usually becomes more harmful than direct injury. When the emotions of the child are disregarded, downplayed, or misinterpreted, the child does not result in concluding that there is something wrong with the caregivers. Rather the growing psyche assimilates a much more agonistic conviction:
“Something about me is wrong.”
This ideology does not stay in childhood. Gradually it becomes incorporated into self-concept the prism through which experiences, relationships, even achievements are perceived. Success feels fragile. Connection feels uncertain. Acceptance feels temporary.
The nervous system is usually on alert even in secure supportive surrounding later in life. It still searches signals of rejection, disapproval, abandonment, not that danger exists, but that it has been taught to expect danger.
This is not oversensitivity. It is the print of a nervous system that is developed under not fulfilled emotional needs, and it is still attempting to defend itself.
6. Why Achievements Don’t Heal the Feeling
Many people carry the belief:
“Once I achieve more, I’ll finally feel enough.”
It is reasonable and even inspirational. However, in practice, success without emotional security does not even cure the sense of inadequacy, it simply does not pay much attention to it.
When success is attained, it may offer temporary relief, confirmation, or power. However, since the belief about the worth is the same, the relief is not permanent. The mind instantly puts the bar higher again, in quest of the next goal, next demonstration, next assurance.
The fundamental dogma is not changed:
- worth is still conditional
- rest still feels undeserved
- success is still so very precarious and can be stolen.
Consequently, even the major achievements can be empty or distressing. Success may create more pressure, rather than confidence, -Now I have to keep it up.
That is why the struggles of many high-achievers are silent:
- chronic anxiety
- emotional emptiness
- imposter syndrome
- fear of being revealed when there is a show of competency.
Achievement is reduced to a treadmill instead of a fulfillment unless the deeper drive behind safety and unconditional self-worth is met.
7. Healing Begins with Safety, Not Self-Improvement
The postulation of non-goodness cannot be cured by being better, more robust or successful. It is cured being made safer in oneself. Once safety is achieved, it is not necessary to earn self-worth anymore.
Psychological healing does not mean forcing the change, but rather letting it gradually loosen. It involves:
- the innermost critic being observed without being obeyed as of course.
- validation of self-correction where self-correction was formerly the rule.
- value to be divided off performance, productivity or approval.
- the perfect regulation of the nervous-system, being peacefully constructed by unity and care.
The inner need to repair, demonstrate or defend starts to reduce as the security level rises. There is no longer a need to ensure that the system remains on high alert.
With time, the internal question is automatically changed. Instead of asking:
“How can I fix myself?”
a more profound, more sympathetic question arises:
What went on that taught my system I was not enough?
This reversal redefines everything not due to a problem being solved but because the individual is not being handled as the problem.
8. You Were Never Broken—You Adapted
A sense of being not good enough is not being weak, failure or lacking. It is evidence of adaptation. What your nervous system did was what it was supposed to do, it learned how to survive in a place where safety, love, consistency or validation was not so sure.
The mind also adapted through alertness, self monitoring and protection. Essays like overthinking, perfectionism, people-pleasing or emotional withdrawal were not weaknesses; they were clever reactions to situations which demanded carefulness.
What used to assist you to cope, no longer need be needed at this moment-but that is no fault in it. It only implies that your system has not yet been demonstrated that there is another way of being safe.
and that can be unlearned that had been learned. Awareness rather than self-blame, compassion rather than judgment, support rather than isolation, and these allow the nervous system to update its beliefs progressively.
You were never broken. You adjusted–and the first step towards healing is to be understood.
A Reframe Worth Remembering
You are not feeling insufficient since you are being underprivileged, broken, or lagging.
You are not good enough since your nervous system has been conditioned to believe that being worthy of living means being worthy of survival, and it was taught at a very young age. It discovered that to be accepted, loved, or safe, one had to be on his or her guard, act, or correct himself.
Such a belief could seem very real as it was needed at one time. But necessity is not truth.
and that belief, as powerful and perennial and persuasive as it may be, is not the truth of yourself. It is an acquired reaction, rather than an identity.
The nervous system, with the help of awareness, compassion and safety may learn something new:
that worth is not earned,
conditioned belonging is not,
and you were always enough.
Frequently Asked Questions (FAQs)
1. Why do I feel “not good enough” even when I’m doing well?
Because this feeling is rarely about ability. It is rooted in how your nervous system learned to associate worth with safety, acceptance, or performance—often early in life.
2. Is feeling “not good enough” a sign of low self-esteem?
Not always. Many people with this feeling are capable and confident in skills but struggle with conditional self-worth, not low ability.
3. Can childhood experiences really affect adult self-worth?
Yes. Early emotional environments shape attachment, nervous-system responses, and core beliefs about worth and belonging.
4. What is conditional love in psychology?
Conditional love occurs when affection or approval depends on behavior, achievement, or emotional compliance rather than being freely given.
5. Why does my inner critic feel so harsh?
The inner critic often develops as a protective mechanism to prevent rejection, shame, or failure—not to hurt you.
6. Is the inner critic bad or harmful?
It becomes harmful when it goes unexamined, but originally it formed to keep you safe in emotionally uncertain environments.
7. Why doesn’t success or achievement make me feel enough?
Because achievement doesn’t address the underlying belief that worth must be earned. Without emotional safety, success feels temporary and fragile.
8. Is this related to imposter syndrome?
Yes. Imposter syndrome often emerges from conditional self-worth and fear of losing belonging despite competence.
9. How does social media increase feelings of inadequacy?
It encourages constant comparison between your real life and others’ curated highlights, activating the brain’s threat system.
10. What role does emotional neglect play?
Emotional neglect teaches the child that their feelings don’t matter, often leading to the belief that something is inherently wrong with them.
11. Is this feeling a trauma response?
It can be. Chronic emotional invalidation, criticism, or inconsistency can leave trauma imprints even without obvious abuse.
12. Can this belief be unlearned?
Yes. With awareness, nervous-system regulation, therapy, and self-compassion, these patterns can change.
13. What does “healing through safety” mean?
It means creating internal and external conditions where the nervous system no longer feels threatened—rather than trying to “fix” yourself.
14. Do I need therapy to heal this?
Therapy can be very helpful, especially trauma-informed or attachment-based approaches, but healing can also begin through awareness and supportive relationships.
15. What’s the most important thing to remember?
You were never broken. You adapted. And adaptation can be gently unlearned.
Written by Baishakhi Das
Counselor | Mental Health Practitioner
B.Sc, M.Sc, PG Diploma in Counseling
References
-
Bessel van der Kolk – The Body Keeps the Score
https://www.besselvanderkolk.com/resources/the-body-keeps-the-score -
John Bowlby – Attachment Theory Overview
https://www.simplypsychology.org/attachment.html -
Kristin Neff – Self-Compassion Research
https://self-compassion.org/the-research/ -
Pete Walker – Complex PTSD & Inner Critic
https://www.pete-walker.com/shrinkingInnerCritic.htm -
Stephen Porges – Polyvagal Theory
https://www.polyvagalinstitute.org/whatispolyvagaltheory -
APA – Trauma and Stress-Related Disorders
https://www.apa.org/topics/trauma
Why Your Brain Won’t Stop Replaying Past Conversations
This topic performs well due to rising searches around men’s mental health, workplace stress, and burnout recovery. Combining emotional insight with practical steps increases engagement and trust.